Building a Master Plan for Aging: Key Elements from States Planning for an Aging Population
summary
This brief, updated from August 2020, highlights states that have a Master Plan for Aging, provides examples of key elements of those plans, and discusses how states without a Master Plan can get started. A Master Plan for Aging is a blueprint that: a) includes planning for 10 or more years; b) is often led by a governor with other executive and legislative leaders; and c) is developed to guide the restructuring of state and local policy, programs, and funding toward aging well in the community.
Date Updated: 10/04/2021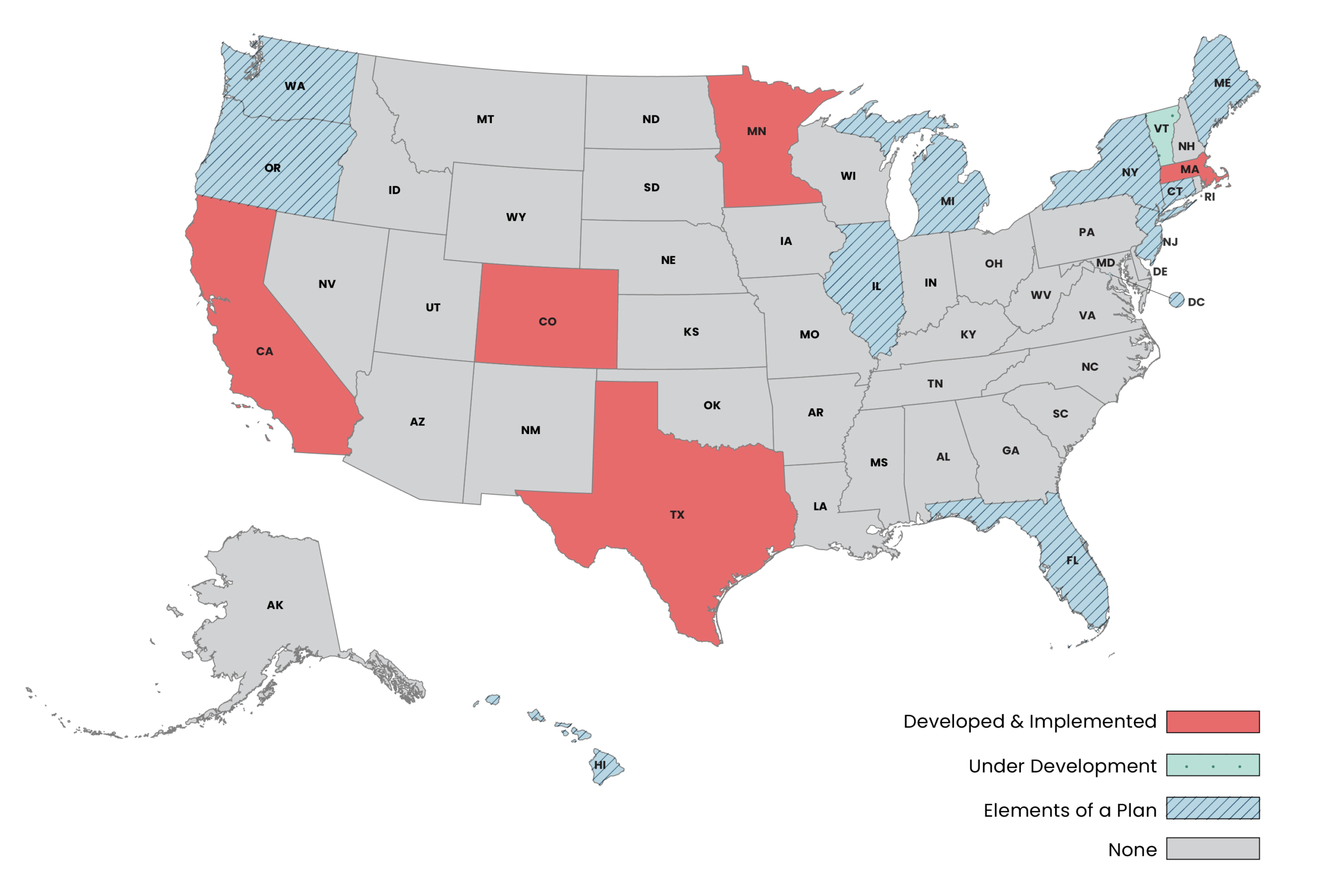
Overview
The United States will reach a turning point in 2030 where 1 in 5 Americans will be age 65 and older; this becomes 1 in 4 by 2060.1 Additionally, the older adult population is growing more racially and ethnically diverse, which requires further attention to prioritize culturally and linguistically competent services to ensure health equity.2 People are also living longer with less access to unpaid family caregiver support than previous generations.3 The coupling of the COVID-19 pandemic and growing recognition of long-standing systemic racism provided powerful examples of these realities, dramatically underscoring the need for an equitable, integrated, community-based health and long-term services and supports (LTSS) infrastructure. States have the option to address these long-standing systemic issues through recent federal funding for home- and community-based services (HCBS) and other social determinants of health.4 All of these developments are shining a spotlight on both challenges and opportunities for reshaping how services are delivered to older adults, people with disabilities, and their family caregivers. States, localities, and communities will experience greater demand for services and prospects for innovation, both of which require farsighted investments in planning.
States have considerable authority to set policy and allocate resources that govern how care and services are organized, delivered, and regulated in a wide range of areas impacting older adults and people with disabilities. According to the AARP LTSS State Scorecard, one of the few common denominators among the highest-performing states is a commitment to a comprehensive plan that guides policy choices and investments to ensure that their aging populations can live with dignity in the settings of their choice. As roughly 70 percent of Americans age 65 and older will need at least some help as they age, a number of forward-thinking states have taken the bold step to develop clearly articulated Master Plans for Aging.5
This brief defines a Master Plan for Aging (Master Plan), and highlights work across states to develop and implement a Master Plan. Drawing from the work in these states, the brief delineates key leadership and structural elements for creating a successful Master Plan while addressing crosscutting themes to guide the planning process. Finally, the brief shows how states without a formal Master Plan effort may already have action in one or more of those essential, structural elements that serve as a pathway for Master Plan development.
What Is a Master Plan for Aging?
A Master Plan for Aging is a blueprint that: a) includes planning for 10 or more years; b) is often led by a governor with other executive and legislative leaders; and c) is developed to guide the restructuring of state and local policy, programs, and funding toward aging well in the community. A successful Master Plan connects the public, private, and independent sectors in renovating systems-based solutions that touch all major areas of the aging life experience (e.g., health, human services, housing, transportation, consumer affairs, employment, income security). It brings visibility to population aging priorities using data and stakeholder input, establishing measurable outcomes to address those priorities while acknowledging infrastructure differences (i.e., provider availability, transportation, internet, and cell service) across urban and rural localities. At its best, a Master Plan is iterative, to be reviewed and updated over time.*
Examples of State Master Plans for Aging
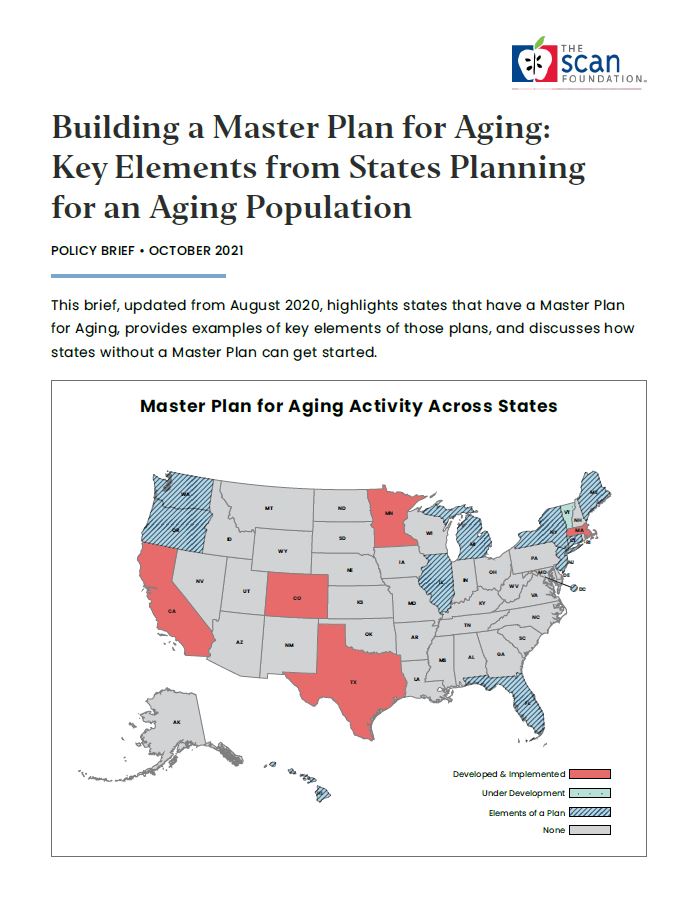
Several states are in various stages of implementing Master Plans. Driven by their respective state-level leadership, Table 1 outlines how California, Colorado, Massachusetts, Minnesota, and Texas have implemented their Master Plans. Each state Master Plan reflects various approaches to addressing system change, such as differences in the range of issues addressed, ranking of priorities, stakeholder involvement, target population, and the extent to which there are accountable and measurable outcomes.
Some of these states also joined AARP’s Age-Friendly Network—a designation recognizing their interest to improve the quality of life for people of all ages through the adoption of policies and programs that address walkable neighborhoods, transportation options, access to key services, support for community engagement, and housing that is affordable and adaptable. California, Colorado, and Massachusetts utilized their robust Master Plans to galvanize state efforts to become Age-Friendly.
Below are descriptions of states with Master Plans, including those meeting Age-Friendly status:
- California’s Master Plan for Aging offers a comprehensive blueprint for cross-sector collaborations to create a California for All Ages by 2030, emphasizing equity and inclusion through person-centered, outcomes-oriented Implementation of the Master Plan is overseen by state leadership with ongoing input from stakeholders on the Disability and Aging Community Living Advisory Committee.6
- Colorado’s Strategic Action Plan on Aging is led by a planning group of state and local policymakers, as well as providers and Updated annually, the plan addresses a range of issues like age-friendly communities, housing, transportation and workforce, which contributed to Colorado acquiring AARP Age-Friendly status. Colorado engaged in extensive stakeholder outreach through its Conversations on Aging project that helped inform the planning process.7
- Massachusetts’ Council to Address Aging was developed to engage stakeholders from the public and private sectors, and leverage technology and innovation. Their blueprint addresses economic security, health care, LTSS, community engagement, and has led to the state acquiring AARP Age-Friendly status and development of ReiMAgine Aging, the Age-Friendly Massachusetts Action Plan.8,9
- Minnesota was one of the earlier states engaged in system planning through its Aging 2030 initiative, with goals centered on a range of issues, including redefining work and retirement; supporting caregivers; and enhancing the use of Building off of this and other initiatives, MN2030 Looking Forward seeks to engage stakeholders in setting LTSS and other priorities that support the life span of all Minnesotans.10
- Texas has been engaged in formal systems planning for an aging population for over a decade. The Aging Texas Well Strategic Plan is reviewed biennially and has evolved to address current issues and future needs. The goals and activities are developed through analysis of current state policy and data. State staff report updates at quarterly advisory committee meetings.11
* All states are required by the Administration for Community Living to submit a State Plan exclusively focused on Older Americans Act funding limited to nutrition and modest community-based support programs. The State Plan goals and outcome measures could be built into or coordinated with similarly focused elements of a broader Master Plan for Aging.
| Table 1: Elements in States with Established Master Plans for Aging | ||||||
| State | Leadership | Rational Priorities | Comprehensive | Stakeholder Involvement | Accountability | AARP Age-Friendly State |
| California | Executive Order N-14-19 calls for a Master Plan for Aging to serve as a blueprint for state government, local communities, private organizations, and philanthropy to work toward an age-friendly California. | Goals are supported by research, data, and stakeholder input. | Goals address:
|
Initial stakeholder engagement included a Stakeholder Advisory Committee, public comment opportunities, community outreach and listening events.
Ongoing stakeholder oversight provided through Disability and Aging Community Living Advisory Committee. |
Progress monitored through the Data Dashboard for Aging and a progress report on the first six months of implementation. | Yes |
| Colorado | HB15-1033 created the Strategic Action Planning Group on Aging, which includes:
|
Goals and recommendations are established using data, and clearly outline agencies and departments involved. | Goals address:
|
Stakeholders provided input through Conversations on Aging. | The report has been updated annually since 2018, with updates included in the 2020 report. The Planning Group will undergo a sunset review in 2022. | Yes |
| Massachusetts | Executive Order 576 created the Governor’s Council to Address Aging in Massachusetts (Council), and called for a plan to make Massachusetts the most age-friendly state for people of all ages. | Recommendations are supported by research, data, and stakeholder input. | Goals address:
|
Feedback gathered through stakeholder meetings, statewide listening sessions, and public comment through an online form. | The Council meets semi-annually to review progress.
ReiMAgine Aging progress report details advancement on the state’s multi- year action plan. |
Yes |
| Minnesota | Minnesota Department of Human Services launched Transform 2010 in partnership with the Minnesota Board on Aging and Department of Health.
The Initiative was later renamed Aging 2030 and built upon to create MN2030. |
Goals are informed by data reported on respective state department websites. | Goals address:
|
Minnesota Board on Aging and state departments of Health and Human Services convened stakeholder meetings across the state. | No measures were developed specific to MN2030. The state adopted performance measures related to specific goals for programs serving people with disabilities and older adults, which are updated annually. | In progress |
| Texas | Executive Order RP-42 mandated the plan be updated every two years under the guidance of the Aging Texas Well Advisory Committee.
All affected agencies and other public entities are required to cooperate fully with implementation. |
Analysis of state policy and data is used to establish goals and activities. | Priority issue areas:
|
The Aging Texas Well Advisory Committee– comprised of academics, providers, community organizations, and consumers – meets quarterly to receive updates from state staff and make recommendations. | The plan is updated biennially.
No measurable outcomes identified, however state staff report progress at quarterly advisory committee meetings. |
No |
Themes to Guide Successful Implementation
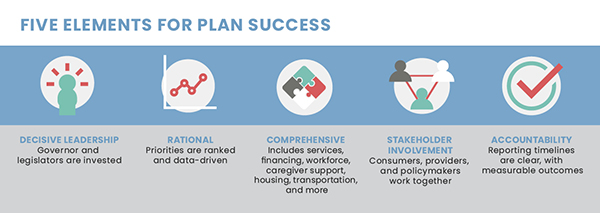
Our review of states’ Master Plan efforts reveals crosscutting themes that impact successful implementation. These themes include intentionally addressing equity at the start, applying and maintaining a person-oriented focus, addressing aging across the life span, and developing cross-sector collaborations (i.e., public, private, and philanthropic). Table 2 highlights how states with established Master Plans apply these themes.
| Table 2: Crosscutting Themes in States with Established Master Plans for Aging | ||||
| State | Equity | Person-Oriented | Aging Across the Life Span | Cross-Sector Collaboration |
| California | The Equity in Aging Advisory Committee advises the governor’s administration on Master Plan implementation. The work group created an equity tool for guidance. | Input gathered from individuals about what matters most as they age was used to guide the Master Plan process.
Recommendations were developed with the person’s experience at the forefront, with reports and updates provided in easy-to-understand language through a variety formats. |
It is a plan for an aging California, recognizing that all Californians are aging. | The public, private, and philanthropic sectors were engaged in the planning process. The Master Plan provides a blueprint for each of the sectors to engage. |
| Colorado | While attention to social determinants of health is evident, a focus on equity is not clearly communicated. Principles of equity and cultural competency were applied to recommendations. | The plan is accessible and presents goals and recommendations in a digestible and user-friendly format. | The aim is to build a Colorado for all by:
|
The Planning Group is comprised of private sector, state departments, higher education, and consumer representatives. |
| Massachusetts | Principles of equity and cultural competency were applied to recommendations. | Uses age-friendly, asset-based language. | The state’s identified values include:
|
The Council is comprised of public, private, and philanthropic sectors intentionally engaging the business and tech communities. Cross-sector engagement to identify goals resulted in solutions from outside state government. |
| Minnesota | The Board of Aging is developing a strategic plan to prioritize diversity, equity, and inclusion (DEI) and bring a DEI lens to all its work. | A common thread throughout the planning has been to ensure older Minnesotans live fulfilling lives.
Public input gathered through Community Conversations informed strategic planning. |
Vision and values express a desire for Minnesota to be a great place to grow old where people of all ages are valued and included in society. | The process is primarily state-driven with some private sector representation on the Governor’s Council for an Age-Friendly Minnesota. |
| Texas | The Health and Human Services Commission (HHSC) plans to review state policies for aging diversity and cultural humility. | Age Well Live Well campaign resources such as toolkits, fact sheets, and infographics are accessible. The campaign aims to provide awareness on aging issues through specialized workshops and promotion of marketing materials. | The Texercise initiative and Age Well Live Well campaign focused on improving outreach to underserved communities. The Texas Talks campaign focused on increasing overall public awareness. | HHSC developed the plan with input from an advisory committee made up of individuals and providers familiar with aging. Cross-sector collaboration is not readily evident. |
States Starting Master Plan Development
Several states are starting to express interest and explore development of a Master Plan. Within the last year, Vermont has taken action to start the development process. Table 3 highlights key leadership actions, stakeholder engagement, and other elements as the basis for its work moving forward.
| Table 3: Elements in States with a Master Plan for Aging Under Development | ||||||
| State | Leadership | Rational Priorities | Comprehensive | Stakeholder Involvement | Accountability | AARP Age-Friendly State |
| Vermont | H611 called for the development of a Master Plan process, which was approved by the Legislature earlier in 2021. | The state uses a variety of reliable data sources to develop outcomes. | Multiple priorities are identified in the Department of Disabilities, Aging and Independent Living (DAIL) Scorecard:
|
DAIL requested public comment on the proposed process and is creating an advisory committee made up of state and local government agencies, the private sector, providers, and academics. | Transparent outcome dashboards provide longitudinal data, sources, and methodologies for replication. | No |
Start with Existing Capacities as a Pathway to Develop a Master Plan for Aging
A number of states have one or more elements of a Master Plan, which can be used as a starting point to engage in a broader planning process to meet the needs of their aging population. Examples include state dashboards reporting program data and outcomes, a variety of social service initiatives addressing the needs of older adults, and/or participation in AARPs Age-Friendly Network—all of which can contribute to and be included in a Master Plan. Table 4 highlights states that do not have a Master Plan but do have one or more elements that could be used as a pathway to develop a Master Plan.
| Table 4: States with Elements that Could Contribute to a Master Plan for Aging | ||||||
| State | Leadership | Rational Priorities | Comprehensive | Stakeholder Investment | Accountability | AARP Age-Friendly Sate |
| Connecticut | Connecticut General Statutes — Title 17B. Social Services Chapter 319Y. Long-Term Care (LTC) —authorizes a planning committee of state administrative staff and legislators to develop a LTC plan. |
The LTC plan establishes goals with short-term and long-term recommendations and has no specified ranking of priorities. |
Priorities focus on provisions for LTSS and rebalancing. | The LTC Advisory Council is comprised of providers, consumers, and advocates. Council provides input to LTC Planning Committee. |
The Plan is released every three years, and outlines goal progress under two themes:
|
No |
| District of Columbia | Initiatives are led by the mayor. | Some goals are supported with data. | Focus areas include:
|
Age-Friendly Task Force includes representation from public, private, and nonprofit sectors; think tanks; media; and local universities. Community members can contribute to implementation as “Agents of Change.” |
Age-Friendly DC progress report includes outcomes dashboard. | Yes |
| Florida | Yes | |||||
| Hawaii | Geographic Information System database and maps inform and track priorities for Age- Friendly Honolulu. |
Executive Office on Aging program performance dashboard provides longitudinal data. |
No | |||
| Illinois | Goals in program-specific plans are supported with data. | A Statewide Movement for Aging Equity engages older adults, caregivers, legislators, academia, and other cross- sector community stakeholders.
The Illinois Aging Together network is under development through an Aging Policy and Advocacy Academy, along with advisory committees made up of cross- sector stakeholders, legislators, and academia. |
No | |||
| Maine | LD 301 encourages Age-Friendly communities (signed into law).
LD 1733 called for a comprehensive state plan and would have established the Director of Aging position to coordinate the planning process if it had passed. Office of Aging and Disability Services and Office of MaineCare Services published recommendations to reform LTSS. |
Some goals are supported with data. | Goals address:
|
The Age-Friendly State Committee is cross-sector with representation from multiple state agencies, the Legislature, private sector, academia, philanthropy, providers, and advocates. | No measurable outcomes noted. | Yes |
| Michigan | Aging and Adult Services Agency reports some data through dashboards and an annual report. | Yes | ||||
| New Jersey | Yes | |||||
| New York | Health Across All Policies/Age-Friendly NY Roadmap Report highlights evidenced- based initiatives. | Suggested goals state agencies could address:
|
Ad hoc committee consisting of representation across state agencies, community partners, local government, and philanthropy. | Yes | ||
| Oregon | Office of Aging and People with Disabilities (APD) have gathered data to inform specific planning and program development (i.e., Oregon LGBTQ+ Older Adult Survey). | APD broad goals include:
|
Age+ and AARP Oregon are gathering stakeholder input through surveys and community conversations. They are also working to build an age-friendly ecosystem, convening leadership toward action. | Oregon Department of Human Services reports some outcomes data (i.e., long-term care and adult protective services). | No | |
Conclusion
A Master Plan provides a blueprint for states and local communities to address what matters most to people as they age—wellness, access to services and supports, and community engagement (e.g., volunteering, employment, recreation). Often, state activities aimed at planning for and addressing the needs of an aging population are fragmented, making the intersections unclear. A Master Plan communicates how various elements come together under one platform as part of a shared state vision. States can take various approaches to plan for an aging population in response to a state’s strengths, capacity, and policy environment. While many states have some form of stakeholder involvement, engaged leadership from the governor is a strong catalyst for implementing a meaningful Master Plan. Additionally, states participating in the AARP Age-Friendly Network can use their efforts as a stepping-stone to develop a broader plan.
Three states (i.e., California, Colorado, and Massachusetts) have found value in the Master Plan processes during COVID-19, using relationships developed through cross-sector collaborations to respond to the needs of older adults, people with disabilities, and their family caregivers. The American Rescue Plan Act of 2021 (ARPA), a COVID-19 relief package includes an increased Federal Medical Assistance Percentage (FMAP) for spending on Medicaid HCBS. States are required to submit an HCBS Spending Plan, which can be updated quarterly, to the Centers for Medicare & Medicaid Services to acquire and use the funds. States with Master Plans were able to draw on Master Plan priorities to guide the development of HCBS spending plans, and leverage this opportunity to support implementation. Overall, a Master Plan maximizes the potential for cross-sector collaborations to develop innovative solutions and shared responsibility for implementation to meet the needs of older people, people with disabilities, and family caregivers—today and in the future.
Download the publication for all visuals and complete references.
Continue Reading
The SCAN Foundation aims to identify models of care that bridge medical care and supportive service systems in an effort to meet people’s needs, values, and preferences. Care coordination is a central component of this vision, which ultimately leads to more person-centered care. This brief outlines The SCAN Foundation’s vision for care coordination in a person-centered, organized system.
This policy brief describes California’s results in the 2014 Long-Term Services and Supports State Scorecard, identifying areas for improvement as well as policy opportunities to transform and improve the state’s system of care.
To succeed in this era of health system transformation, plans and providers bearing risk – in an accountable care organization (ACO) for example – will need strategies for managing a broad array of care needs for high-risk beneficiaries across multiple settings of care. Download this fact sheet to learn more.