What Matters Most: Essential Attributes of a High-Quality System of Care for Adults with Complex Care Needs (Full Report)
summary
Adults with complex care needs are currently often served by a number of providers and systems that do not talk to each other or coordinate efforts, making it difficult for individuals to receive high-quality care. Efforts to transform delivery systems and associated quality measurements for this vulnerable population are also fragmented. The SCAN Foundation convened a working group to develop consensus on the Essential Attributes of a high-quality system of care that supports system transformation and evaluation. This full report includes the abbreviated literature review of existing frameworks.
Date Updated: 08/15/2016Introduction
Currently, adults with complex care needs are often served by a number of providers and systems that do not talk to each other or coordinate efforts, making it difficult for individuals to receive high-quality care. Efforts to transform delivery systems and associated quality measurements for this vulnerable population are also fragmented across multiple organizations and institutions, as well as state and federal governments.*
As various health systems move toward streamlining services and care for adults with complex care needs, a number of critical goals must be met. The individuals served and their family/caregivers must be at the center of system evolution. Delivery systems must work together as a simplified, easy to navigate, cohesive whole. Health care and supportive services should be tailored to each individual’s unique circumstances, preferences, and goals for living a full and meaningful life. Health and well-being, including living independently, are essential and need to encompass the social, non-medical components of home- and community-based services.+ Quality measurement across payers and delivery systems needs to capture the effectiveness of services that help with function, independence, and assure the receipt of necessary and desired supportive services in the least restrictive setting possible.
In pursuit of these goals, The SCAN Foundation (Foundation) convened a working group of diverse experts representing the interests of adults with complex care needs. Federal officials working on relevant programs participated as ex-officio members, as did representatives from other foundations with related interests. (See Appendix A – Working Group and Ex-Officio Participant List)
The goal of the working group was to develop consensus on the Essential Attributes of a high-quality system of care that supports system transformation and evaluation, and is from the vantage point of adults with complex care needs.
Multiple frameworks exist or are in development, but there is currently no single statement of what a delivery system must have to effectively serve adults with complex care needs. The working group recognized the need to address this gap and identify what matters most for quality systems supporting this vulnerable population. Through a consensus process, the group developed an overarching goal statement:
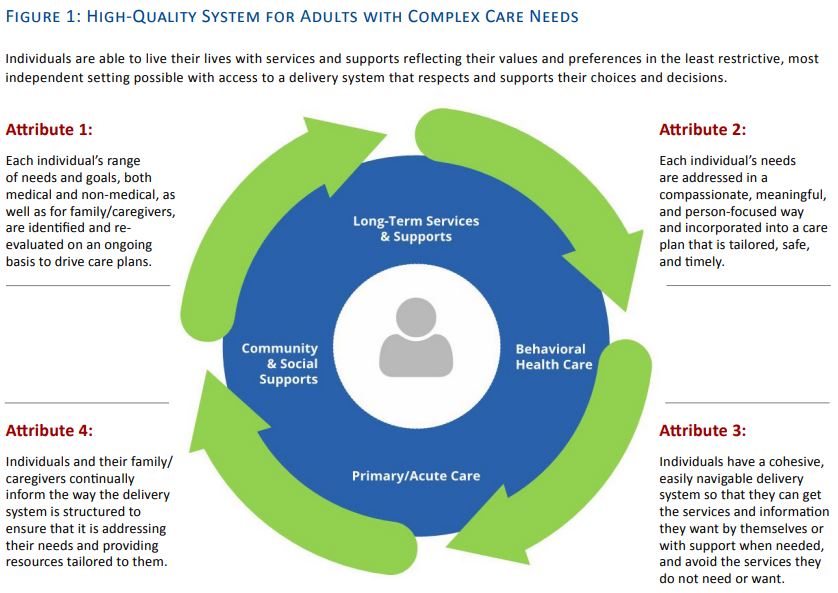
Individuals are able to live their lives with services and supports reflecting their values and preferences in the least restrictive, most independent setting possible with access to a delivery system that respects and supports their choices and decisions.
The working group also developed four Essential Attributes of a high-quality system of care that supports system transformation and evaluation, as well as core elements in the functioning of such
a system. These Essential Attributes build on a large body of existing expert frameworks and are intended to help guide future efforts to transform delivery systems and develop quality measures capturing individuals’ goals, preferences, and desired outcomes.
The Essential Attributes aim to inform and support the diverse array of stakeholders working to improve care for adults with complex care needs. These include the individual, their family/ caregivers, quality measurement organizations, state and federal policymakers and organizations, advocacy and consumer groups, service providers, health plans and delivery systems, and others that are part of and have an interest in health care and long-term services and supports (LTSS)
delivery systems for this population.
At the outset, the working group recognized several issues and concerns. The group identified the need to address the structure of health care, LTSS, and social service delivery systems in order to comprehensively provide quality support. There was consensus that fragmented systems and funding streams need to be seamless, offering flexibility in benefit design so that those with complex care needs can have those needs met by a quality system designed around the individual. The group highlighted that family/caregivers are major providers of LTSS to individuals with complex care needs, and therefore delivery systems should acknowledge their unique role while assessing and addressing their needs with appropriate information, training, respite care, and other supportive services tailored to their values and preferences.
However, while the working group recognized that adults with complex care needs belong to many distinct subpopulations, this paper does not define these subpopulations. Instead, it identifies what matters most to individuals and their family/caregivers: the Essential Attributes of a high quality system. In addition, while the group realized that resources and sustainability (including the ability of delivery systems to be discerning in how they deploy available resources) are important, these issues were not the focus of this effort, since other public- and private-sector entities are currently addressing them through other initiatives.
Methodology
Project Components and Working Group
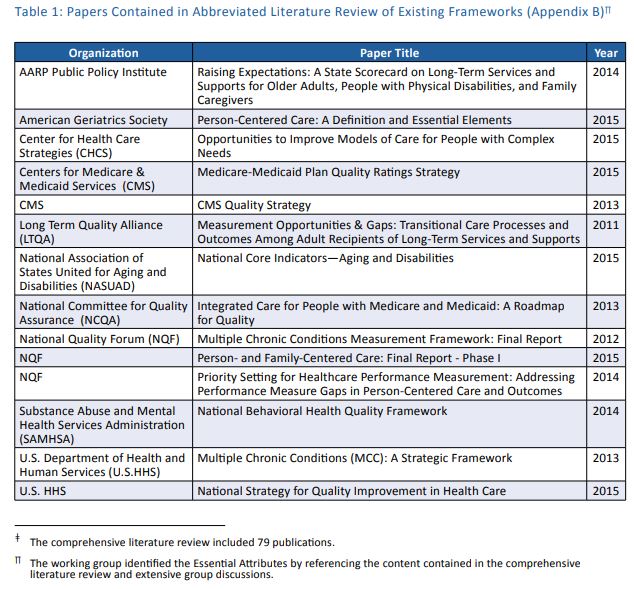
This project consisted of three main components. First, a comprehensive literature review was conducted, in which the large body of ongoing work by many organizations, collaborations, and governments was examined, and quality frameworks and measurements for serving people with complex care needs were identified (along with related gray literature).ǂ Next, three meetings of the working group were held, with ex-officio members participating. In addition, individual interviews with all working group members and selected ex-officio members were conducted.
The working group drew program and quality expertise from quality measurement organizations, state governments, and consumer advocates, and there was representation of health plans. A selection of leaders from the federal government and health care foundations, serving as exoficio members, provided input into the working group process and product. The Foundation also commissioned expert facilitation and technical assistance from the Alliance for Health Reform and Health Management Associates.
Process
The literature review, working group consensus process, and interviews identified existing definitions of “complex needs populations” and other terms used by state and federal governments for publicly financed health care as well as by health care institutions, health plans, and consumer organizations. Review of “person-centered care,” “family-centered care,” and “quality of life” definitions informed the working group effort to focus on individuals with complex needs and their goals, preferences, and choices. The literature review and interviews identified the
importance of developing and formalizing approaches to considering the needs of family/caregivers as essential people who support and self-activate adults with complex care needs. Family members/caregivers enable such individuals to remain stable and connected to community, family, and friends. Support for family/caregivers is now recognized as a key component of a high-performing LTSS system. Further review and discussion emphasized identifying the social determinants of health (e.g., housing, transportation, income, health literacy, nutrition) and the role and responsibility of the health care system in addressing them. Utilizing all of this rich content through an iterative process, the working group articulated the Essential Attributes.
Existing Definitions of Adults with Complex Needs
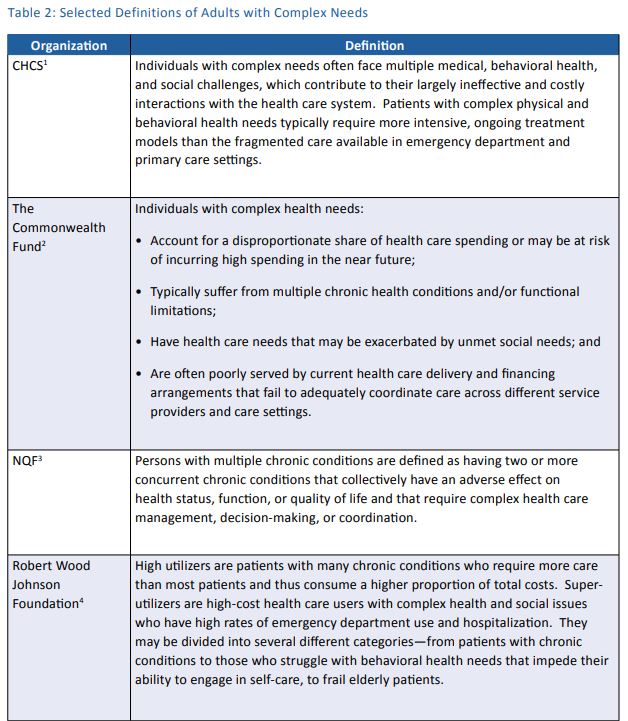
Various definitions of adults with complex needs are employed and applied differently across contexts. Table 2 provides selected definitions is use today and shows their variability. For articulating the Essential Attributes, the working group considered all of these to create a single definition of adults with complex care needs.
Essential Attributes of a High-Quality System for Adults with Complex Care Needs
The working group articulated four Essential Attributes of a high-quality delivery system serving and supporting adults with complex care needs. Collectively, these Essential Attributes represent the milestones that, when regularly monitored and measured, can track progress toward the overarching goal. They are intended to help guide future efforts to transform delivery systems and develop quality measures that capture individuals’ goals, preferences, and desired outcomes. Figure 1 (see page 10) depicts the connected continuum of the four Essential Attributes around the individual and the care and supports they receive. Key definitions precede Figure 1 and the detailed elements of each Essential Attribute.5
Key Definitions
The following two definitions were developed to guide the working group consensus process:
- Adults with complex care needs: Individuals having two or more mental and/or physical chronic conditions, and additional functional limitations that collectively have an effect on health status and quality of life.
- Essential Attribute: A feature regarded as a characteristic or inherent part of care delivery by providers serving adults with complex care needs, which affects its success or failure. Below are definitions for terms used in Figure 1, which are drawn from existing sources:
- Behavioral health care: Refers to services that encompass prevention and promotion of emotional health; prevention of mental and substance use disorders, substance use, and
related problems; treatments and services for mental and substance use disorders; and recovery support.6 - Community and social supports: Refers to services and supports that are not LTSS that promote independence, well-being, self-determination, social connectedness and community inclusion in meaningful, desired activities of individuals with complex needs, supporting each individual to remain in his/her home and/or community.7 Community and social supports include items such as housing, transportation, employment, and education.
- Family/caregiver: Broadly defined, refers to any relative, partner, friend or neighbor, as well as paid caregivers, who has a significant personal relationship with, and who provides a broad range of assistance for an adult with complex care needs.8,9
- LTSS: Refers to assistance with activities of daily living (ADLs) and instrumental activities of daily living (IADLs) provided in homes, community residences, or institutional settings to people with complex needs who cannot perform these activities on their own due to a physical, cognitive, or chronic health condition that is expected to continue for an extended period of time, typically 90 days or more. LTSS also include supports provided to family members and other unpaid caregivers.10
- Primary/acute care: Primary care refers to care provided by physicians, nurse practitioners, physician assistants or other qualified health professionals specifically trained for and skilled
in comprehensive first contact and continuing care for persons with any undiagnosed sign, symptom, or health concern. Primary care services include health promotion, disease prevention, health maintenance, counseling, patient education, diagnosis and treatment of acute and chronic illnesses.11 Acute care refers to a type of primary care that includes all promotive, preventive, curative, rehabilitative, or palliative actions whose primary purpose is to improve health and whose effectiveness largely depends on time-sensitive and, frequently, rapid intervention.12
ATTRIBUTE 1: Each individual’s range of needs and goals, both medical and non-medical, as well as for family/caregivers, are identified and re-evaluated on an ongoing basis to drive care plans.
Delivery systems:
- Appropriately and adequately identify adults with complex care needs;
- Assess each individual’s needs in a comprehensive and holistic way, to the extent desired by the individual;
- Identify each individual’s goals, preferences, strengths, and values by a care team member with whom the individual and family/caregiver feel comfortable;
- Share information about the individual’s goals, preferences, strengths, and values with the individual’s entire care team;
- Use assessment approaches that take into account an individual’s entire history, its impact on his/her health, and support well-being and strengths (i.e., recovery-oriented and trauma-informed);
- Promote community integration, social supports, and care coordination, including opportunities for self-directed care to the greatest extent feasible; and
- Identify family/caregivers’ needs and the natural supports and home- and community based resources that enable them to provide assistance aligned with the individual’s needs and preferences, and ensure they get the training/support they require.
ATTRIBUTE 2: Each individual’s needs are addressed in a compassionate, meaningful, and person-focused way and incorporated into a care plan that is tailored, safe, and timely.
Delivery systems:
- Support the individual and his/her family/caregivers to guide the care plan to the greatest extent feasible;
- Use a collaborative partnership approach to decision-making with the individual and his/her family/caregivers;
- Develop care plans that address daily living needs;
- Empower each individual with tools and strategies to promote his/her strengths and self-management of care within the care plan; and
- Use individual choice and priorities to help guide the most appropriate medical and social support strategy that is accessible and aligned with both the individual’s values and the family/caregivers’ needs.
ATTRIBUTE 3: Individuals have a cohesive, easily navigable delivery system so that they can get the services and information they want by themselves or with support when needed, and avoid the services they do not need or want.
Delivery systems:
- Ensure high-quality, coordinated, integrated, and accessible services that meet an individual’s full set of care needs (including, primary care, behavioral health care and substance use disorder treatment, LTSS, and technological assistance) in the most appropriate setting;
- Provide timely information on the benefits, costs, and risks of care and service options that individuals and their family/caregivers can understand and evaluate alongside their needs, values, and preferences in order to make decisions;
- Ensure that the individual is at the center of decision-making regarding care and services, and a full partner with their entire care team;
- Support timely, uninterrupted care and service delivery via an accountable primary point of contact who understands the complete picture of the individual’s needs and has the authority and services and supports to connect the individual and family/caregivers to needs and services, as well as grievances and appeals processes across settings and systems;
- Ensure that care teams effectively communicate with the individual, family/caregivers, and each other to support continuous, coordinated, and integrated care;
- Acknowledge that circumstances and environment affect individuals’ ability to navigate care and services, and tailor support to reflect these circumstances; and
- Provide culturally competent care and services tailored to each individual, as well as their family/caregiver, and the individual’s strengths, health literacy, language proficiency, and social/environmental circumstances.
ATTRIBUTE 4: Individuals and their family/caregivers continually inform the way the delivery system is structured to ensure that it is addressing their needs and providing resources tailored to them.
Delivery systems:
- Solicit and are responsive to ongoing collective input from individuals and the family/ caregivers served;
- Provide ways for individuals and their family/caregivers to raise issues outside of the delivery system’s formal grievance and appeal channels (i.e., hold regular local forums to solicit input);
- Support meaningful input by individuals and their family/caregivers for continuous improvement; and
- Evolve based on individuals’ and family/caregivers’ input into design, implementation, and evaluation to ensure the system is responsive to all individuals being served and their family/caregivers.
Essential Attributes Context
While not explicitly referenced in the Essential Attributes, the following aspects of systems are prevalent in the literature and of note when considering a high-quality system.
- Affordability: Systems must be affordable in order to be accessible by individuals and their family/caregivers. The attributes do not directly address this issue, but note that “accessibility” includes affordability.
- Publicly-financed health system fiscal constraints: Literature and working group members noted the cost and difficulty of creating expectations that may be in conflict with fiscal realities for publicly-financed health care.
- Social determinants of health: Spectrums of viewpoints exist regarding which determinants the health care system should address and prioritize. Within the working group, consensus existed that the health system should be identifying certain determinants (e.g., housing, nutrition, transportation, financial well-being, education, health literacy) and taking them into consideration when addressing and supporting individual’s needs, goals, and preferences. A divide exists as to what the health care system should be held accountable for addressing, what it is responsible for, and to what extent. The working group relayed that fiscal constraints must be considered and there is need to clearly delineate the responsibilities of the health care system versus other social service systems.
- Person-centered care: In order to be very specific about what is essential, based on feedback from working group members the attributes did not use the term “person centered care,” or “person- and family-centered care.” Instead, more explicit words are used to describe what a person-focused system should seek to achieve from the perspective of an adult with complex care needs and their family/caregivers, where appropriate.
- Quality of life: In order to be specific about what is essential, based on feedback from working group members the attributes did not use the term “quality of life.” Instead, the attributes more specifically describe what adults with complex care needs seek and prefer in order to live their lives according to their choices
Summary Reflections
The consensus of the working group and resulting Essential Attributes articulate what matters most for high-quality care from the perspective of an adult with complex care needs. The Essential Attributes seek to describe critical quality elements of a system regardless of the specific subpopulation being served. The working group expressed that models of care and interventions must be tailored to the individuals living with complex care needs and system elements must work together as a seamless – and to the greatest extent possible – single delivery system that is easy to understand and navigate. The Essential Attributes are intended to help guide future efforts to develop quality measures that capture the goals, preferences, and desired life outcomes of adults
with complex care needs.
Download the publication for all visuals and complete references.
Continue Reading
The SCAN Foundation aims to identify models of care that bridge medical care and supportive service systems in an effort to meet people’s needs, values, and preferences. Care coordination is a central component of this vision, which ultimately leads to more person-centered care. This brief outlines The SCAN Foundation’s vision for care coordination in a person-centered, organized system.
This policy brief describes California’s results in the 2014 Long-Term Services and Supports State Scorecard, identifying areas for improvement as well as policy opportunities to transform and improve the state’s system of care.
To succeed in this era of health system transformation, plans and providers bearing risk – in an accountable care organization (ACO) for example – will need strategies for managing a broad array of care needs for high-risk beneficiaries across multiple settings of care. Download this fact sheet to learn more.


