Innovating for Medicare Beneficiaries
Medicare beneficiaries with chronic conditions and daily living challenges struggle to navigate a complex system of care whether they have both Medicare and Medi-Cal, or are Medicare only. While states do not have fiscal responsibility for the Medicare program, there is an opportunity to influence care delivery and enhance approaches to improve access and coordinate medical and nonmedical services in support of community living.
Fact Sheets
We surveyed Californians age 55 and older to better understand their health care needs and experiences.
The Challenge
States are responsible for implementing the Medicaid program and therefore have traditionally focused efforts on building infrastructure for Medicaid beneficiaries. Policymakers and stakeholders are now recognizing the importance of building Medicare capacity to support Medicare-only beneficiaries with complex care needs as well. Many of these individuals are part of the “forgotten middle” – older adults who do not have sufficient financial resources to pay for health care and long-term services and supports (LTSS), yet do not meet eligibility requirements for many government-funded programs, including Medicaid.
Similarly, dually eligible beneficiaries face challenges in accessing streamlined services, i.e., fragmentation in how LTSS services are delivered across both systems of care.
The Opportunity
States can position themselves to improve equitable access to high-quality care and services for the Medicare population. Establishing the infrastructure needed to build and sustain Medicare capacity over time will help states develop the expertise to create innovative models of care. There is a need for:
- State-level policy leadership to create a person-centered system of care for dual-eligible adults and Medicare-only beneficiaries with complex care needs; and
- Medicaid agency staff to develop knowledge of Medicare’s evolving landscape of policies, regulations, and market activity.
Ensuring Success Within the Office of Medicare Innovation and Integration
The California Department of Health Care Services (DHCS) Office of Medicare Innovation and Integration (OMII) was established in 2021 and tasked with expanding the health and human service focus beyond Medicaid to improve health outcomes, quality, affordability, and equity for all Medicare beneficiaries in California (6.6 million), including those that are dually eligible (1.6 million).
In partnership with DHCS OMII, we have supported efforts to build a better understanding of California’s Medicare population and inform policy and programs. Developed with ATI Advisory, an ongoing series of chartbooks provides information on the demographics, needs, and health care experiences of California’s Medicare beneficiary population.
- Profile of the California Medicare Population details key characteristics of the state’s Medicare beneficiaries to help inform the future efforts.
- Culturally and linguistically responsive programs and services are critical to addressing disparities and improving experience of care. Cultural and Linguistic Demographics of the California Medicare Population includes information about language and birthplace demographics.
- California’s older Medicare beneficiaries with income just above the Medi-Cal income eligibility limit (near dual) have a similar demographic profile to people dually eligible for Medicare and Medi-Cal. They also have higher rates of disability and less access to social supports than those with higher incomes. Profile of Older Californians: Medicare Beneficiaries Near Income Eligibility for Medi-Cal highlights the needs of this near-dual population.
- Supplemental Benefits in Medicare Advantage (MA) Plans in California provides information on the California MA landscape, highlighting a subset of MA plans, including D-SNPs, and the prevalence of specific supplemental benefits provided throughout the state. A related factsheet, 2023 Medicare Advantage Supplemental Benefits offers a comparison of MA supplemental benefit offerings in California with Medi-Cal benefits.
- Chronic Conditions Experienced by Californians with Original Medicare in 2021 provides information on the chronic conditions most commonly experienced by Californians with Original Medicare and related Medicare spending. This data provides a lens into who might benefit from policies, programs, and services that target specific chronic conditions.
Survey of California’s Medicare Beneficiaries and Fact Sheets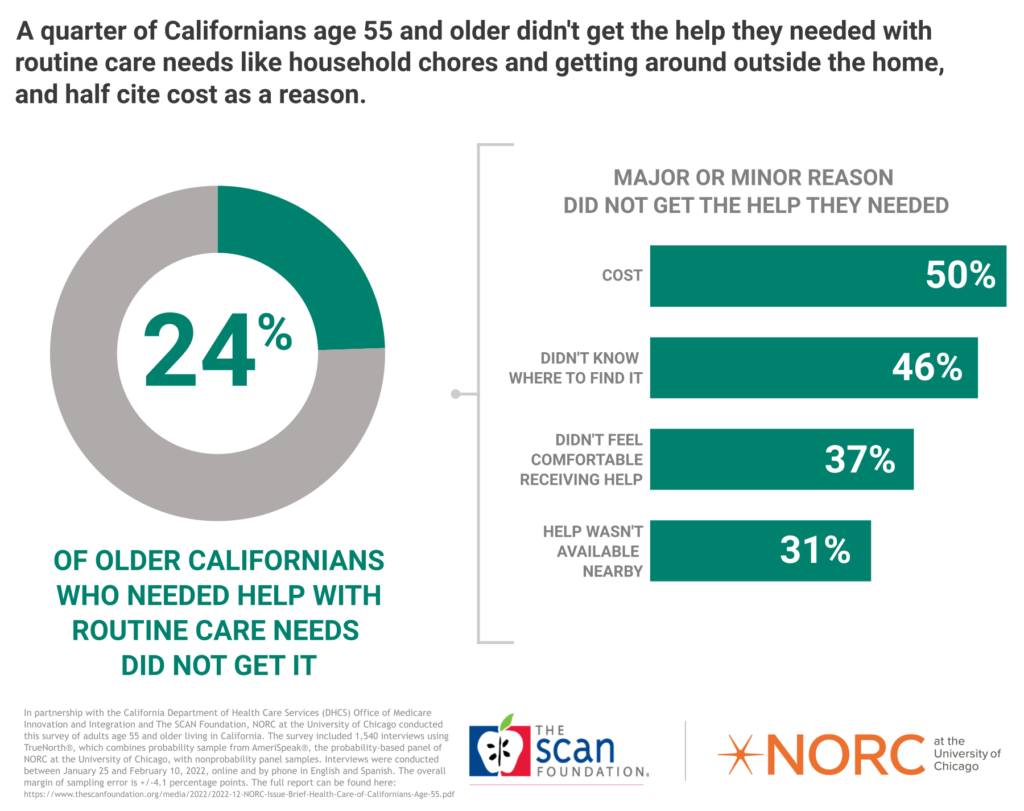
The National Opinion Research Center (NORC) at the University of Chicago conducted a 2022 survey on the health care needs and experiences, and opinions of 1,540 Californians age 55 and older. The data reflects the population by age, race and ethnicity, gender, education, and region. View the related fact sheets.
Building Medicare Savvy Among State Medicaid Staff
With our support alongside Arnold Ventures and The Commonwealth Fund, the Center for Health Care Strategies (CHCS) launched the Medicare Academy in October 2022 to support Medicaid agencies focused on building the Medicare capacity needed to advance integrated care and build the infrastructure needed to sustain Medicare capacity over time.
The 10-month long Academy is working with eight states – Colorado, Hawaii, Maine, North Carolina, Texas, Virginia, Washington, and Wisconsin – to build the Medicare knowledge they need to:
- Develop and oversee Medicare-Medicaid integration programs; and
- Engage in longer-term policy and program refinement.
Our Thought Partners
ATI Advisory
ATI Advisory is a research and advisory services firm that helps health care and government leaders transform care delivery for older adults with complex needs and their families.
Center for Health Care Strategies
Center for Health Care Strategies is a nonprofit dedicated to improving health care quality for low-income people, those with chronic illnesses and disabilities, vulnerable older adults, and racially and ethnically diverse populations who are experiencing disparities.
Chapman Consulting
Chapman Consulting is a consulting firm with expertise in federal and state health policy, researching and evaluating the current landscape and its impacts to provide comprehensive and actionable strategies.
National Opinion Research Center
The National Opinion Research Center (NORC) at the University of Chicago is one of the world’s premier social science research organizations. NORC’s mission is to conduct rigorous research on key social problems and policy issues.

